The microbes in your vagina do a lot to protect you against potentially dangerous infections. If you’re trying to get pregnant, you want them on your team.
So, you’re thinking about starting a family. First of all, congratulations! This is an exciting time—but of course, it can also be an incredibly stressful and overwhelming one too. Between tracking your cycle, deciding on the best prenatal, and carefully timing the deed, there’s a whole lot to consider, and a whole lot that falls out of your control.
We want to put some of the power back into your hands—and that’s why we’re taking a minute to demystify the vaginal microbiome’s role in pregnancy. Here’s how the microscopic world in your vagina helps lay the foundation for new life.

Science with us—nerdy reads for your inbox biome1
1By signing up, you consent to receive Seed emails.
The Role of the Vaginal Microbiome During Pregnancy
Your vagina is home to roughly 10 billion microorganisms—from bacteria to archaea and fungi.1,2 This may sound alarming at first, but it’s actually pretty amazing. When functioning as it should, this vast, microscopic landscape helps shield you from infection, keep your vagina comfortable, and more.3
Within the past decade, scientists have taken a closer look at this vaginal microbiome (VMB) and how it changes over time. It turns out that the makeup of your VMB can shift depending on where you are in your cycle, what medications you’re taking, and even how often you’re having sex.4-6 Needless to say, the VMB seems to change throughout pregnancy and postpartum too.7
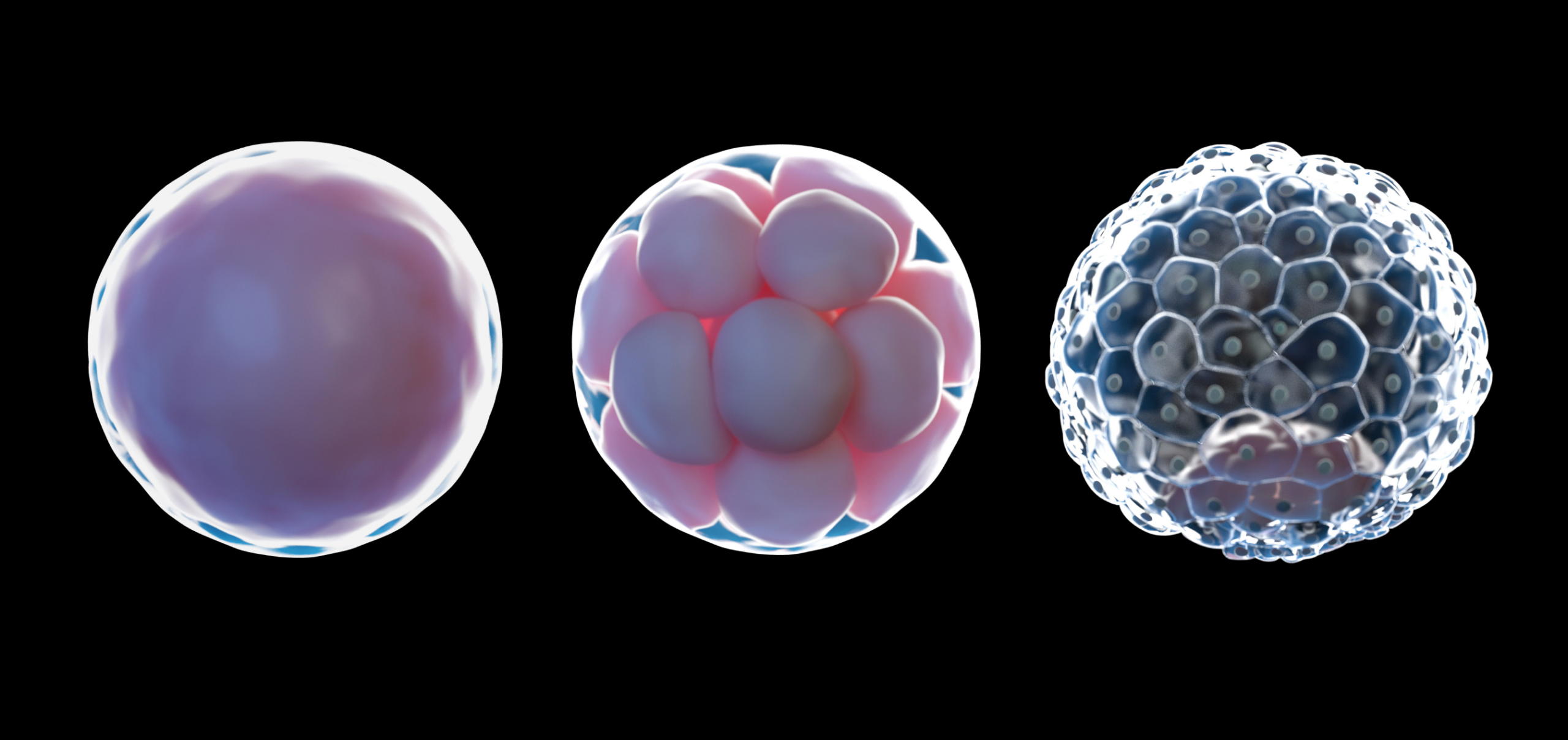
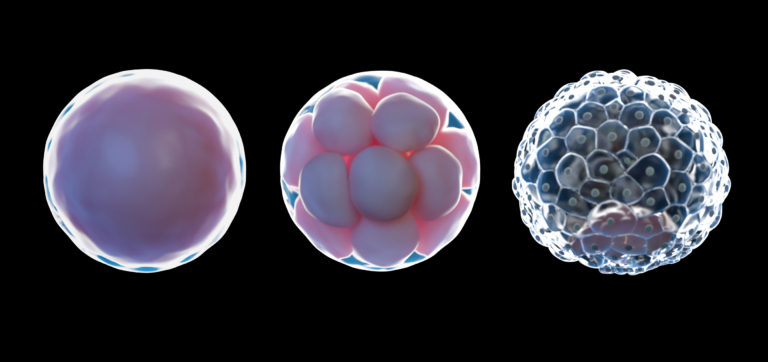
We’ve already done a deep, deep dive into how the VMB impacts fertility but to quickly recap: bacteria from the vaginal microbiome may impact the composition of the cervix—a gatekeeping barrier between the vagina and the uterus that is protected by a thick mucus lining.8 Changes in cervical mucus consistency and quality can impact sperm motility and their ability to reach and fertilize an egg.9
Once a sperm passes through the cervix and fertilizes an egg, it must be implanted into the uterine lining. The vaginal microbiome may lend a proverbial hand in this process too. A disrupted VMB may be associated with worse in vitro fertilization (IVF) outcomes and conditions caused by vaginal microbiome disruption (such as bacterial vaginosis) have been tied to increased rates of implantation failure and pregnancy complications.10,11
As pregnancy progresses, increasing levels of estrogen and progesterone can facilitate a shift towards a more stable VMB that’s dominated by Lactobacillus—a bacterial genus that produces lactic acid and protects against infection.7,12 Having a protective vaginal microbiome through pregnancy seems to help fend off infections that may pose risks to both the mother and developing fetus.7,13 Plus, research suggests that protective Lactobacillus species like Lactobacillus crispatus may be associated with a decreased risk of preterm birth.3,14
While these are fascinating early findings, researchers are still trying to untangle the exact role the VMB plays during different stages of pregnancy.
OK, So What Does This Mean for Me?
If there’s a possibility you may want to try to become pregnant one day, tending to your vaginal microbiome can only help—and you can get started right away.
That’s because harboring bacterial species like L. crispatus will be beneficial regardless of your pregnancy status.3,15 Research shows that having a vaginal microbiome that is dominated by this species can be protective against BV, certain STIs, and even gynecological cancer.16-18
An optimal VMB will look different for everyone, and you can shape yours by limiting microbial disruptors like sugary, high-fat foods and introducing protective microbial strains into the vagina using a well-formulated vaginal probiotic.19-21 Be sure to look for one that contains strains that are native to the vagina and have been clinically validated to restore (and maintain) a strong VMB. As always, consult your healthcare provider before starting a new regimen.
Limiting your exposure to certain pollutants also seems to pay off for your microbes. Some, such as particulate matter in the air, are tough to avoid, while others, like cigarette smoke, fall more squarely within your control.22,23 Reducing the use of unnecessary antibiotics and practicing microbiome-friendly sex (clean those toys!) can also help shape a strong, resilient vaginal ecosystem.5,24
The Life-Giving Power of Your Microbial Entourage
A Lactobacillus-dominant vaginal microbiome, especially one with plenty of Lactobacillus crispatus bacteria, has been shown to support key conception and pregnancy outcomes. The more you can do to prepare your microbial entourage early, the better set up your reproductive environment will be—for yourself and any other future residents of your uterus.
Citations
- Chen, C., Song, X., Wei, W., Zhong, H., Dai, J., Lan, Z., Li, F., Yu, X., Feng, Q., Wang, Z., Xie, H., Chen, X., Zeng, C., Wen, B., Zeng, L., Du, H., Tang, H., Xu, C., Xia, Y., . . . Jia, H. (2017). The microbiota continuum along the female reproductive tract and its relation to uterine-related diseases. Nature Communications, 8(1). https://doi.org/10.1038/s41467-017-00901-0
- Reid, G. (2017). Therapeutic opportunities in the vaginal microbiome. Microbiology Spectrum, 5(3). https://doi.org/10.1128/microbiolspec.bad-0001-2016
- France, M., Alizadeh, M., Brown, S. E., Ma, B., & Ravel, J. (2022). Towards a deeper understanding of the vaginal microbiota. Nature Microbiology, 7(3), 367–378. https://doi.org/10.1038/s41564-022-01083-2
- Eschenbach, D. A., Thwin, S. S., Patton, D. L., Hooton, T. M., Stapleton, A. E., Agnew, K., Winter, C., Meier, A., & Stamm, W. E. (2000). Influence of the normal menstrual cycle on vaginal tissue, discharge, and microflora. Clinical Infectious Diseases, 30(6), 901–907. https://doi.org/10.1086/313818
- Lin, Y. P., Chen, W. C., Cheng, C. M., & Shen, C. J. (2021). Vaginal pH value for clinical diagnosis and treatment of common vaginitis. Diagnostics (Basel, Switzerland), 11(11), 1996. https://doi.org/10.3390/diagnostics11111996
- Lewis, F. M. T., Bernstein, K. T., & Aral, S. O. (2017). Vaginal microbiome and its relationship to behavior, sexual health, and sexually transmitted diseases. Obstetrics and Gynecology, 129(4), 643–654. https://doi.org/10.1097/AOG.0000000000001932
- MacIntyre, D. A., Chandiramani, M., Lee, Y. S., Kindinger, L., Smith, A., Angelopoulos, N., Lehne, B., Arulkumaran, S., Brown, R., Teoh, T., Holmes, E., Nicoholson, J. K., Marchesi, J. R., & Bennett, P. R. (2015). The vaginal microbiome during pregnancy and the postpartum period in a European population. Scientific Reports, 5(1). https://doi.org/10.1038/srep08988
- Dong, M., Dong, Y., Bai, J., Li, H., Ma, X., Li, B., Wang, C., Li, H., Qi, W., Wang, Y., Fan, A., Han, C., & Xue, F. (2023). Interactions between microbiota and cervical epithelial, immune, and mucus barrier. Frontiers in Cellular and Infection Microbiology, 13. https://doi.org/10.3389/fcimb.2023.1124591
- Katz D. F. (1991). Human cervical mucus: Research update. American Journal of Obstetrics and Gynecology, 165(6 Pt 2), 1984–1986. https://doi.org/10.1016/s0002-9378(11)90559-6
- Haahr, T., Jensen, J. S., Thomsen, L., Duus, L., Rygaard, K., & Humaıdan, P. (2016). Abnormal vaginal microbiota may be associated with poor reproductive outcomes: A prospective study in IVF patients. Human Reproduction, 31(4), 795–803. https://doi.org/10.1093/humrep/dew026
- Ravel, J., Moreno, I., & Simón, C. (2021). Bacterial vaginosis and its association with infertility, endometritis, and pelvic inflammatory disease. American Journal of Obstetrics and Gynecology, 224(3), 251–257. https://doi.org/10.1016/j.ajog.2020.10.019
- Romero, R., Hassan, S. S., Gajer, P., Tarca, A. L., Fadrosh, D. W., Nikita, L., Galuppi, M., Lamont, R. F., Chaemsaithong, P., Miranda, J., Chaiworapongsa, T., & Ravel, J. (2014). The composition and stability of the vaginal microbiota of normal pregnant women is different from that of non-pregnant women. Microbiome, 2(1). https://doi.org/10.1186/2049-2618-2-4
- Chen, X., Lu, Y., Chen, T., & Li, R. (2021b). The female vaginal microbiome in health and bacterial vaginosis. Frontiers in Cellular and Infection Microbiology, 11. https://doi.org/10.3389/fcimb.2021.631972
- Fettweis, J. M., Serrano, M. G., Brooks, J. P., Edwards, D. J., Girerd, P. H., Parikh, H. I., Huang, B., Arodz, T. J., Edupuganti, L., Glascock, A. L., Xu, J., Jimenez, N. R., Vivadelli, S. C., Fong, S. S., Sheth, N. U., Jean, S., Lee, V., Bokhari, Y. A., Lara, A. M., . . . Buck, G. A. (2019). The vaginal microbiome and preterm birth. Nature Medicine, 25(6), 1012–1021. https://doi.org/10.1038/s41591-019-0450-2
- Amabebe, E., & Anumba, D. (2018). The vaginal microenvironment: The physiologic role of Lactobacilli. Frontiers in Medicine, 5. https://doi.org/10.3389/fmed.2018.00181
- Abdelmaksoud, A. A., Koparde, V. N., Sheth, N. U., Serrano, M. G., Glascock, A. L., Fettweis, J. M., Strauss, J. F., Buck, G. A., & Jefferson, K. K. (2016). Comparison of Lactobacillus crispatus isolates from Lactobacillus-dominated vaginal microbiomes with isolates from microbiomes containing bacterial vaginosis-associated bacteria. Microbiology (Reading, England), 162(3), 466–475. https://doi.org/10.1099/mic.0.000238
- Nardini, P., Palomino, R. a. Ñ., Parolin, C., Laghi, L., Foschi, C., Cevenini, R., Vitali, B., & Marangoni, A. (2016). Lactobacillus crispatus inhibits the infectivity of Chlamydia trachomatis elementary bodies, in vitro study. Scientific Reports, 6(1). https://doi.org/10.1038/srep29024
- Champer, M., Wong, A. M., Champer, J., Brito, I., Messer, P. W., Hou, J. Y., & Wright, J. D. (2017). The role of the vaginal microbiome in gynaecological cancer. BJOG, 125(3), 309–315. https://doi.org/10.1111/1471-0528.14631
- Lebeer, S., Ahannach, S., Gehrmann, T., Wittouck, S., Eilers, T., Oerlemans, E., Condori, S., Dillen, J., Spacova, I., Donck, L. V., Masquillier, C., Allonsius, C. N., Bron, P. A., Van Beeck, W., De Backer, C., Donders, G., & Verhoeven, V. (2023). A citizen-science-enabled catalogue of the vaginal microbiome and associated factors. Nature Microbiology, 8(11), 2183–2195. https://doi.org/10.1038/s41564-023-01500-0
- Neggers, Y. H., Nansel, T. R., Andrews, W. W., Schwebke, J. R., Yu, K. F., Goldenberg, R. L., & Klebanoff, M. A. (2007). Dietary intake of selected nutrients affects bacterial vaginosis in women. The Journal of Nutrition, 137(9), 2128–2133. https://doi.org/10.1093/jn/137.9.2128
- Hertz, F. B., Holm, J. B., Pallejá, A., Björnsdóttir, M. K., Mikkelsen, L. S., Brandsborg, E., & Frimodt-Møller, N. (2022). Vaginal microbiome following orally administered probiotic. APMIS. Acta Pathologica, Microbiologica Et Immunologica Scandinavica, 130(10), 605–611. https://doi.org/10.1111/apm.13261
- Oyebode, I. H., Just, A. C., Ravel, J., Elovitz, M. A., & Burris, H. H. (2023). Impact of exposure to air pollution on cervicovaginal microbial communities. Environmental Research, 233, 116492. https://doi.org/10.1016/j.envres.2023.116492
- Nelson, T. M., Borgogna, J. C., Michalek, R. D., Roberts, D. W., Rath, J. M., Glover, E. D., Ravel, J., Shardell, M., Yeoman, C. J., & Brotman, R. M. (2018). Cigarette smoking is associated with an altered vaginal tract metabolomic profile. Scientific Reports, 8(1). https://doi.org/10.1038/s41598-017-14943-3
- Plummer, E. L., Vodstrcil, L. A., Fairley, C. K., Tabrizi, S. N., Garland, S. M., Law, M. G., Hocking, J. S., Fethers, K. A., Bulach, D. M., Murray, G. L., & Bradshaw, C. S. (2019). Sexual practices have a significant impact on the vaginal microbiota of women who have sex with women. Scientific Reports, 9(1), 19749. https://doi.org/10.1038/s41598-019-55929-7