What exactly is bacterial vaginosis? What causes it? And how can you treat it so it doesn’t come back? We answer all of it and more in this shame-free guide to BV.
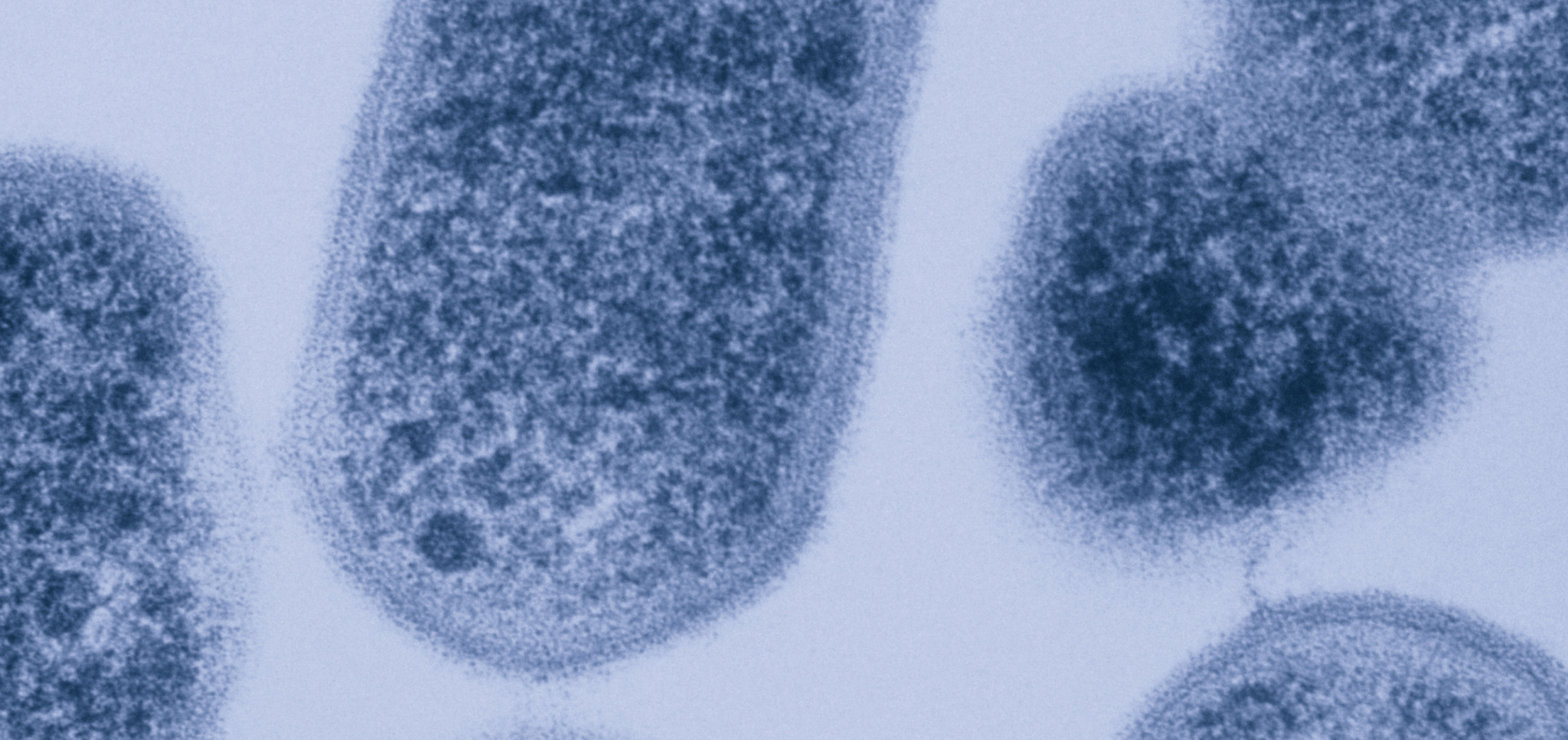
Pictured above: Gardnerella vaginalis (a species of bacteria that can cause bacterial vaginosis) under a microscope.
From a young age, many of us are taught that vaginas should be demure. They shouldn’t smell, they shouldn’t itch, and they most certainly shouldn’t produce fluid. It’s easy to see then why bacterial vaginosis (BV)—an imbalance of the vaginal microbiome (VMB) that can lead to a fishy odor and abnormal discharge—has become so stigmatized.
With 21 million women in the U.S. currently harboring BV (whether they know it or not), a shame-free guide is long overdue.1 So, what exactly is BV? What causes it? And how can you treat it so it doesn’t come back? Let’s dig in.
What is Bacterial Vaginosis and How Do I Know If I Have It?
Bacterial vaginosis is a lot like a high school house party (stick with me here). When adults are present, the festivities can stay relatively calm and uneventful. But the second the parents leave, kids let loose and invite their friends, who invite more friends, and before you know it things can get…messy.
Similarly, without protective bacteria supervising the vaginal microbiome, pathogens can come to the party and unleash all kinds of chaos.
In this analogy, Lactobacillus species are the parents: these bacteria are responsible for producing lactic acid (which establishes a moderately acidic pH in the vagina) and bacteriocins (which inhibit the growth of certain bacterial strains).2 Without dominant Lactobacillus species, the VMB becomes more susceptible to the spread of unwanted house guests.3
While researchers used to think that one bacterial species, Gardnerella vaginalis, caused BV, we know there are multiple BV-associated pathogens, including species of Prevotella, Mobiluncus, and more.4 Many of these bacteria naturally live in the vagina—it’s only when they grow in excess that they can cause imbalances (also known as “dysbiosis”).
“Ultimately, BV is not caused by the mere presence of the potential pathogens (which is common) but rather by their unrestrained increase in number, often reaching cell counts that are 100 – 1000 fold above the normal bacterial levels of the vagina,” explains one article in The Journal of Applied Microbiology.5
Bacterial vaginosis (BV) is the most common cause of abnormal vaginal discharge in women of childbearing age and affects nearly one-third of reproductive-aged women at any given time—though at least half of them will be asymptomatic.6-8
Those who do present with symptoms tend to have an increase in vaginal discharge that is white or gray, watery, or otherwise abnormal for them. This discharge often has a foul or fishy odor, and is especially prominent after sexual intercourse.9 In some cases, those with BV might also experience itchiness around the vulva.8
If you notice any of these symptoms, it’s best not to self-diagnose, since other conditions like yeast infections and STIs can present similarly. Your doctor can make the official diagnosis after analyzing your discharge and measuring your vaginal pH to see if it falls outside the standard range (anything above ~4.5 can be indicative of BV).7,9
It’s best to flag symptoms quickly, as BV can be a risk factor for other vaginal issues. After being diagnosed with bacterial vaginosis, women have an increased risk of acquiring STIs like chlamydia and gonorrhea.9 BV pathogens have been linked to pregnancy complications, including a higher risk of preterm birth, and lower birthweight in some studies.9,10 There is also some evidence that BV-associated organisms are associated with pelvic inflammatory disease, which can cause damage to the reproductive tract and infertility.7,11
But again, BV is an extremely common condition that doesn’t usually cause serious complications—you just want to get it under control early if you can.12
Potential Causes and Contributors to BV
Despite BV’s prevalence, we’re still not sure exactly what leads to the bacterial imbalance. It’s likely that it doesn’t have one specific cause but can be set off by a confluence of factors, including:
- Soap and douching: Washing out your vagina with soap has been shown to reduce the amount of lactobacilli in the VMB, potentially increasing one’s risk of BV. The vagina is self-cleaning and any attempt to manually wash it or flush it out with water (douching) disrupts healthy vaginal microbes, setting the scene for opportunistic, BV-causing pathogens. Sexual hygiene also seems to play a role in BV development—we’ll dig deeper into that below.9,12,13
- IUDs: Using a copper IUD may slightly increase your risk of BV compared to other forms of birth control, according to some studies.14,15 Researchers suspect this could be due to the fact that copper IUDs can increase bleeding.16 Since menstrual blood has a slightly higher pH than the vagina, it could temporarily lead to microbial disruption. A study published last year also found that copper ions hinder the growth of Lactobacillus crispatus (a highly protective type of Lactobacillus) in vitro and promote the growth of Lactobacillus iners (which are more volatile), as well as elevate concentrations of cytokines that signal vaginal mucosal inflammation, setting the scene for pathogen overgrowth.15
- Cigarette smoking: Some research has linked smoking cigarettes to a decrease in protective bacteria and a higher risk of BV—potentially because of BPDE, a chemical in cigarette smoke that might deplete lactobacilli concentrations.17,18
It’s important to acknowledge that the composition of the vaginal microbiome naturally ebbs and flows, leaving us more prone to dysbiosis during certain periods of menstruation and menopause.19,20 Ethnicity also seems to play a role in VMB profile.21 All of this to say, if you’re diagnosed with BV, know that it’s common, treatable, and not at all “your fault.”
The Complicated Role of Sex in BV
BV is not a sexually transmitted infection (say it louder for people in the back!). STIs happen when foreign bacteria get introduced into the vagina, whereas BV is an overgrowth of native vaginal bacteria. It can occur even if you have never had vaginal sex, or haven’t had it recently.22
Instead, BV has been called a “sexually enhanced” infection, since sex can create the right microbial conditions for BV to develop.23 Having frequent unprotected sex or sex with multiple partners is often cited as a risk factor for BV infection, thanks to the way sex alters the natural balance of bacterial flora within the vagina.9,23 There is also some research to show that having anal sex before vaginal intercourse might be associated with BV risk.24
However, if you’re worried about BV, you don’t need to swear off sex altogether. Using condoms and staying on top of sexual hygiene (think: cleaning your hands and toys prior to the fun) can go a long way in reducing your risk of infection following intercourse.25
BV Treatment and Prevention
If you go to the doctor with BV, chances are you’ll be prescribed an antibiotic (likely clindamycin or metronidazole) to be taken orally or vaginally. While medications are effective at clearing the initial infection, they don’t do much to restore balance in the VMB long-term—one reason why recurrent infections are quite common.7 An estimated 50% of women who take antibiotics for BV experience a recurring infection within three to six months (!).26
Sometimes, BV pathogens can also develop what’s known as a biofilm—in essence, a shield that protects them from the body’s defense mechanisms. This could be another reason why BV can be so difficult to get rid of for good.7,27
Researchers are now looking into how repopulating the VMB with Lactobacillus species can address the root cause of BV infection (and prevent it from returning in the future).28,29
Some strategies that can up your lactobacilli count include avoiding disruptors of beneficial bacteria (think: unnecessary antibiotics, cigarette smoke, douching, and soaps) and practicing good sexual hygiene. Some early research also suggests that diets that are high in fat and low in vitamins A, C, D, E, β-carotene, folate, and calcium may increase the risk of BV.30,31 Taking a well-formulated probiotic vaginally, on the other hand, can help colonize the VMB with beneficial bacteria like L. crispatus.
Whatever you do, don’t take treatment into your own hands. There is no evidence to show that DIY remedies like yogurt-soaked tampons help cure BV—and they might make things worse. Consult your doctor to find a solution that works for you.
Imagining a World Without BV
BV is a common vaginal imbalance that brings way too many people way too much shame. Emerging research on the vaginal microbiome reveals the intricate microbial networks that cause this fickle infection—and gives us clues about how to kick it for good.
Citations
- Koumans, E. H., Sternberg, M., Bruce, C., McQuillan, G., Kendrick, J., Sutton, M., & Markowitz, L. E. (2007). The prevalence of bacterial vaginosis in the United States, 2001–2004; Associations with symptoms, sexual behaviors, and reproductive health. Sexually Transmitted Diseases, 34(11), 864–869. https://doi.org/10.1097/olq.0b013e318074e565
- France, M., Alizadeh, M., Brown, S. E., Ma, B., & Ravel, J. (2022). Towards a deeper understanding of the vaginal microbiota. Nature Microbiology, 7(3), 367–378. https://doi.org/10.1038/s41564-022-01083-2
- Amabebe, E., & Anumba, D. (2018). The vaginal microenvironment: The physiologic role of lactobacilli. Frontiers in Medicine, 5. https://doi.org/10.3389/fmed.2018.00181
- Hay, P. E. (2002). Bacterial Vaginosis as a mixed infection. In K. A. Brogden & J. M. Guthmiller (Eds.), Polymicrobial Diseases (Chap. 7). ASM Press. https://www.ncbi.nlm.nih.gov/books/NBK2495/
- Turovskiy, Y., Noll, K. S., & Chikindas, M. L. (2011). The aetiology of bacterial vaginosis. Journal of Applied Microbiology, 110(5), 1105–1128. https://doi.org/10.1111/j.1365-2672.2011.04977.x
- Hay P. (2017). Bacterial vaginosis. F1000Research, 6, 1761. https://doi.org/10.12688/f1000research.11417.1
- Abbe, C., & Mitchell, C. (2023). Bacterial vaginosis: A review of approaches to treatment and prevention. Frontiers in Reproductive Health, 5. https://doi.org/10.3389/frph.2023.1100029
- Coudray, M. S., & Madhivanan, P. (2020). Bacterial vaginosis-A brief synopsis of the literature. European Journal of Obstetrics, Gynecology, and Reproductive Biology, 245, 143–148. https://doi.org/10.1016/j.ejogrb.2019.12.035
- Kairys, N., & Garg, M. (2023, July 4). Bacterial vaginosis. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK459216/
- Hillier, S. L., Nugent, R. P., Eschenbach, D. A., Krohn, M. A., Gibbs, R. S., Martín, D. H., Cotch, M., Edelman, R., Pastorek, J. G., & Rao, A. P. (1995). Association between bacterial vaginosis and preterm delivery of a low-birth-weight infant. The New England Journal of Medicine, 333(26), 1737–1742. https://doi.org/10.1056/nejm199512283332604
- Jennings, L. K., & Krywko, D. M. (2023, March 13). Pelvic inflammatory disease. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK499959/
- World Health Organization: WHO & World Health Organization: WHO. (2023b, August 16). Bacterial vaginosis. https://www.who.int/news-room/fact-sheets/detail/bacterial-vaginosis#
- Lokken, E., Manguro, G., Abdallah, A. N., Ngacha, C., Shafi, J., Kiarie, J., Jaoko, W., Srinivasan, S., Fiedler, T. L., Munch, M. M., Fredricks, D. N., McClelland, R. S., & Balkus, J. E. (2019). Association between vaginal washing and detection of Lactobacillus by culture and quantitative PCR in HIV-seronegative Kenyan women: A cross-sectional analysis. Sexually Transmitted Infections, 95(6), 455–461. https://doi.org/10.1136/sextrans-2018-053769
- Peebles, K., Kiweewa, F. M., Palanee‐Phillips, T., Chappell, C. A., Singh, D., Bunge, K., Naidoo, L., Makanani, B., Jeenarain, N., Reynolds, D. J., Hillier, S. L., Brown, E. R., Baeten, J. M., Balkus, J. E., Mtn, & Team, A. S. (2020). Elevated risk of bacterial vaginosis among users of the copper intrauterine device: A prospective longitudinal cohort study. Clinical Infectious Diseases, 73(3), 513–520. https://doi.org/10.1093/cid/ciaa703
- Brown, B. P., Feng, C., Tanko, R. F., Jaumdally, S. Z., Bunjun, R., Dabee, S., Happel, A. U., Gasper, M., Nyangahu, D. D., Onono, M., Nair, G., Palanee-Phillips, T., Scoville, C. W., Heller, K., Baeten, J. M., Bosinger, S. E., Burgener, A., Passmore, J. S., Heffron, R., & Jaspan, H. B. (2023). Copper intrauterine device increases vaginal concentrations of inflammatory anaerobes and depletes lactobacilli compared to hormonal options in a randomized trial. Nature Communications, 14(1), 499. https://doi.org/10.1038/s41467-023-36002-4
- Madden, T., Grentzer, J. M., Secura, G. M., Allsworth, J. E., & Peipert, J. F. (2012). Risk of bacterial vaginosis in users of the intrauterine device. Sexually Transmitted Diseases, 39(3), 217–222. https://doi.org/10.1097/olq.0b013e31823e68fe
- Nelson, T. M., Borgogna, J. C., Michalek, R. D., Roberts, D. W., Rath, J. M., Glover, E. D., Ravel, J., Shardell, M., Yeoman, C. J., & Brotman, R. M. (2018). Cigarette smoking is associated with an altered vaginal tract metabolomic profile. Scientific Reports, 8(1). https://doi.org/10.1038/s41598-017-14943-3
- Holdcroft, A. M., Ireland, D. J., & Payne, M. S. (2023). The vaginal microbiome in health and disease-what role do common intimate hygiene practices play?. Microorganisms, 11(2), 298. https://doi.org/10.3390/microorganisms11020298
- Eschenbach, D. A., Thwin, S. S., Patton, D. L., Hooton, T. M., Stapleton, A. E., Agnew, K., Winter, C., Meier, A., & Stamm, W. E. (2000). Influence of the normal menstrual cycle on vaginal tissue, discharge, and microflora. Clinical Infectious Diseases, 30(6), 901–907. https://doi.org/10.1086/313818
- Muhleisen, A. L., & Herbst-Kralovetz, M. M. (2016). Menopause and the vaginal microbiome. Maturitas, 91, 42–50. https://doi.org/10.1016/j.maturitas.2016.05.015
- Ravel, J., Gajer, P., Abdo, Z., Schneider, G. M., Koenig, S. S., McCulle, S. L., Karlebach, S., Gorle, R., Russell, J., Tacket, C. O., Brotman, R. M., Davis, C. C., Ault, K., Peralta, L., & Forney, L. J. (2011). Vaginal microbiome of reproductive-age women. Proceedings of the National Academy of Sciences of the United States of America, 108 Suppl 1(Suppl 1), 4680–4687. https://doi.org/10.1073/pnas.1002611107
- Yen, S., Shafer, M.-A., Moncada, J., Campbell, C. J., Flinn, S. D., & Boyer, C. B. (2003). Bacterial vaginosis in sexually experienced and non–sexually experienced young women entering the military. Obstetrics & Gynecology, 102(5, Part 1), 927-933.
- Amabebe, E., & Anumba, D. O. C. (2022). Mechanistic insights into immune suppression and evasion in bacterial vaginosis. Current Microbiology, 79(3), 84. https://doi.org/10.1007/s00284-022-02771-2
- Cherpes, T. L., Hillier, S. L., Meyn, L. A., Busch, J. L., & Krohn, M. A. (2008). A delicate balance: Risk factors for acquisition of bacterial vaginosis include sexual activity, absence of hydrogen peroxide-producing lactobacilli, black race, and positive herpes simplex virus type 2 serology. Sexually Transmitted Diseases, 35(1), 78–83. http://www.jstor.org/stable/44969361
- Hutchinson, K. B., Kip, K. E., & Ness, R. B. (2007b). Condom use and its association with bacterial vaginosis and bacterial vaginosis-associated vaginal microflora. Epidemiology, 18(6), 702–708. https://doi.org/10.1097/ede.0b013e3181567eaa
- Chow, K., Wooten, D., Annepally, S., Burke, L., Edi, R., & Morris, S. R. (2023). Impact of (recurrent) bacterial vaginosis on quality of life and the need for accessible alternative treatments. BMC Women’s Health, 23(1), 112. https://doi.org/10.1186/s12905-023-02236-z
- Machado, D., Castro, J., Palmeira-de-Oliveira, A., Martinez-de-Oliveira, J., & Cerca, N. (2016). Bacterial vaginosis biofilms: Challenges to current therapies and emerging solutions. Frontiers in Microbiology, 6, 1528. https://doi.org/10.3389/fmicb.2015.01528
- Falagas, M. E., Betsi, G. I., & Athanasiou, S. (2007). Probiotics for the treatment of women with bacterial vaginosis. Clinical Microbiology and Infection, 13(7), 657–664. https://doi.org/10.1111/j.1469-0691.2007.01688.x
- Webb, L. (2021). Probiotics for preventing recurrent bacterial vaginosis. Journal of the American Academy of Physician Assistants, 34(2), 19–22. https://doi.org/10.1097/01.jaa.0000731484.81301.58
- Neggers, Y. H., Nansel, T. R., Andrews, W. W., Schwebke, J. R., Yu, K. F., Goldenberg, R. L., & Klebanoff, M. A. (2007). Dietary intake of selected nutrients affects bacterial vaginosis in women. The Journal of Nutrition, 137(9), 2128–2133. https://doi.org/10.1093/jn/137.9.2128
- Thoma, M. E., Klebanoff, M. A., Rovner, A. J., Nansel, T. R., Neggers, Y. H., Andrews, W., & Schwebke, J. R. (2011b). Bacterial vaginosis is associated with variation in dietary indices. The Journal of Nutrition, 141(9), 1698–1704. https://doi.org/10.3945/jn.111.140541