A decades-long exploration of the gut-brain axis may have implications for how we treat anxiety disorders in the not-so-distant future.

The human brain, with its intricate systems of neurotransmitters and receptors, is dauntingly complicated. But in a lot of ways, it’s like a big tongue.
We often think in words, but consider what it’s like to touch a crystal of salt to your tongue: It doesn’t automatically cause the words “that’s salty” to cross your mind. Instead, the activation of those taste buds is a direct line into your conscious experience, altering your psychological state. Tasting salt is a state of mind, in the most literal sense of the phrase, and any words we use to categorize or catalog the experience are subsequent to that.
Now, imagine that—instead of five kinds of taste buds—you have 500, and your body is capable not only of sensing and translating these chemical signals the way your tongue does, but also of producing them in response to something you see, or even in response to a thought inside your own head. If you can imagine that, you’ve got a pretty decent picture of what a brain is like.
These 500 types of “taste buds” are your brain’s neurotransmitter receptors, and the chemicals that land on them (the “salt”) are the neurotransmitters themselves. The two most fundamental neurotransmitters are glutamate (which excites the neurons it lands on, making it easier for them to be activated) and GABA (which calms them down and makes it harder). These two neurotransmitters are “downstream” of many of the more familiar ones like serotonin, dopamine, and melatonin—each of which might have glutamate-enhancing activity in one part of the brain, and GABA-enhancing activity in another.
And just as the distinct flavors in a meal blend with one another (and with other sensations like smell) to make a unique experience which is greater than the sum of its parts, it’s the simultaneous sensation of all those myriad neurochemicals that coalesces into your conscious experience of the world. The balance and flux of them throughout your day forms the landscape that guides your train of thought through the dense thicket of junctions that is your brain. Each moment is a mouthful, a meal. How does this one taste?
In this lies the root of the intense curiosity around meditation, drugs, and other altered states of mind—which is inherent not only to humans, but to nearly all intelligent animals.1 The impulse to seek out ways to deliberately alter that neurochemical milieu is an expression of the desire not to simply eat at the table of life, but to cook for ourselves. And any chef worth their salt earns that distinction through experimentation, tasting ingredients and seasonings in isolation, then together, to develop a sense of what a dish “needs.” This isn’t purely metaphor, either: In kitchens around the world, you’ll find the brain’s primary excitatory neurotransmitter, glutamate, on the shelf as its monosodium salt: MSG.
In fact, the connection from what’s in your gut to what’s going on in your brain is potentially the most promising avenue we have for altering a state of mind for the better. Nowhere is this more apparent than in the decades-long search for the natural mechanism of anti-anxiety drugs like Xanax. We now know that the path leads to the gut microbiome, but to understand how and why, you’ll need to appreciate the journey scientists took to get there.

Science with us—nerdy reads for your inbox biome1
1By signing up, you consent to receive Seed emails.
The Accidental Discovery of “Natural Xanax”
Whether in the kitchen or in the brain, we learn about complex systems by toying with them. As a result, the history of neuroscience and the history of psychopharmacology (the study of drugs and their impact on the brain) are inextricably intertwined. Take endorphins, for example, which are largely responsible for the regulation of pain and pleasure. After an injury like a burn to the finger, the body produces and releases these neurotransmitters, enabling us to partially “tune out” the signals from the burnt tissue, because—while acute pain is useful in alerting us to damage or distress—it doesn’t do much good to be continuously reminded “still burnt!”
This is the feedback system that we are “hacking into” when we take opioid painkillers like codeine or morphine, which work by landing on and activating the same receptors as endorphins.2 But morphine, extracted from the poppy plant, was in use long before we began to understand the brain, and this history is written into the name we gave the system: “Endorphin” is a portmanteau, a contraction of “endogenous (i.e. ‘from within’) morphine.”
This pattern, where a drug that works by mimicking a natural neurotransmitter was in use long before we understood the system that it acts on, is repeated again and again in the history of neuroscience. The endocannabinoid system, the system that we “hack” when we use cannabis, is another example, although its various functions (including immunity, memory, appetite, and fertility) are far less straightforward than those of the endorphins.
The pattern continued even into the modern era, when new drugs began to be developed through chemistry, rather than discovered in nature. In the late 1950s, the first-ever benzodiazepine was synthesized (by accident, as it happens) and found to have powerful sedative and anti-anxiety properties, while lacking many of the side effects that plagued similar drugs in use at the time.
Within a decade of their introduction, benzodiazepines—a class of drug which now includes Valium, Xanax, Klonopin, and numerous others—were among the most highly prescribed drugs in the world, in spite of the fact that scientists had very little idea how they work. It wasn’t until the late 1970s that researchers began to identify the molecular mechanism by which benzodiazepines exert their anti-anxiety effect.3,4
Part of the reason this took some time to discover is that benzodiazepines don’t work by substituting for a neurotransmitter the same way that morphine mimics the endorphins, or THC subs in for the endocannabinoids. Instead, it was found that benzodiazepines work by attaching to an “accessory” site on the GABA receptor, changing its structure in such a way that the GABA which is already there at the receptor becomes more effective at its job.5 To extend the cooking analogy, it’s like adding a spice to your dish that brings out the other ingredients’ natural sweetness, rather than adding sugar.
But this still left a mystery: Did the scientist who created the first benzodiazepine just get incredibly lucky, accidentally creating a molecule which has no natural equivalent, but which happens to tease the brain’s proteins into a shape that enhances GABA signaling without disturbing anything else? It seems unlikely. But if not, then what chemical from the human brain is supposed to land on the spot that Xanax and Valium hit, acting as the natural equivalent of the “volume” knob on our GABA receptors? In short: We’ve identified the natural molecules in the human body that serve as endorphins and endocannabinoids—but what are the “endo-benzos”?
It’s a question that’s still not fully answered to this day, but the first tantalizing clues as to its solution came in the resolution of another long-standing medical mystery: hepatic coma.
The Key Difference Between “Anti-Xanax” and “Un-Xanax”
When a person is in end-stage liver failure, typically one of the last things to happen is that they slip into a relatively peaceful, sleep-like state referred to as “hepatic coma.” For a long time, nobody understood exactly why, but in the late 1980s, a scientist at the National Institutes of Health (NIH) in the U.S. noticed something funny: The brainwave patterns of rabbits in hepatic coma looked remarkably similar to the brainwave patterns that showed up in animals sedated with heavy doses of benzodiazepines.6
Intrigued, he devised a simple experiment: The comatose rabbits were given a dose of a drug called flumazenil.
The rabbits woke up. They weren’t exactly happy about being awake, because their livers were still shot and their brains were swimming in ammonia as a result—but the fact that they had woken up was itself an incredible thing, because flumazenil has a very specific mode of action. It only works as an antidote to benzodiazepines.7 If a person has overdosed on something like Xanax, flumazenil can save their life, the same way the drug naloxone (or “Narcan”) can bring someone back from a deadly fentanyl overdose. But flumazenil is not anti-Xanax, only un-Xanax: Giving it to a healthy person won’t make them anxious, the same way that giving Narcan to someone healthy doesn’t cause them pain. Here, then, was a sign that there are “endo-benzos,” and that they were somehow involved in causing hepatic coma.
Not long after, other research groups exploring this enigma began to report equally remarkable findings. One reported finding N-desmethyl-diazepam, a molecule nearly identical to Valium, in the brains of people who couldn’t have possibly taken the drug, because they had died and their brains had been “banked” decades prior—before Valium was even invented.8
The implication—that the body naturally makes a chemical almost identical to Valium—sparked a minor uproar in the scientific literature. Some groups reported that they had replicated the finding, while others asserted that their methods must be sloppy, or their equipment contaminated.9,10 They asserted that “natural Valium” was impossible on general principle, for the simple reason that Valium and the related chemical being reported both contain a chlorine atom.
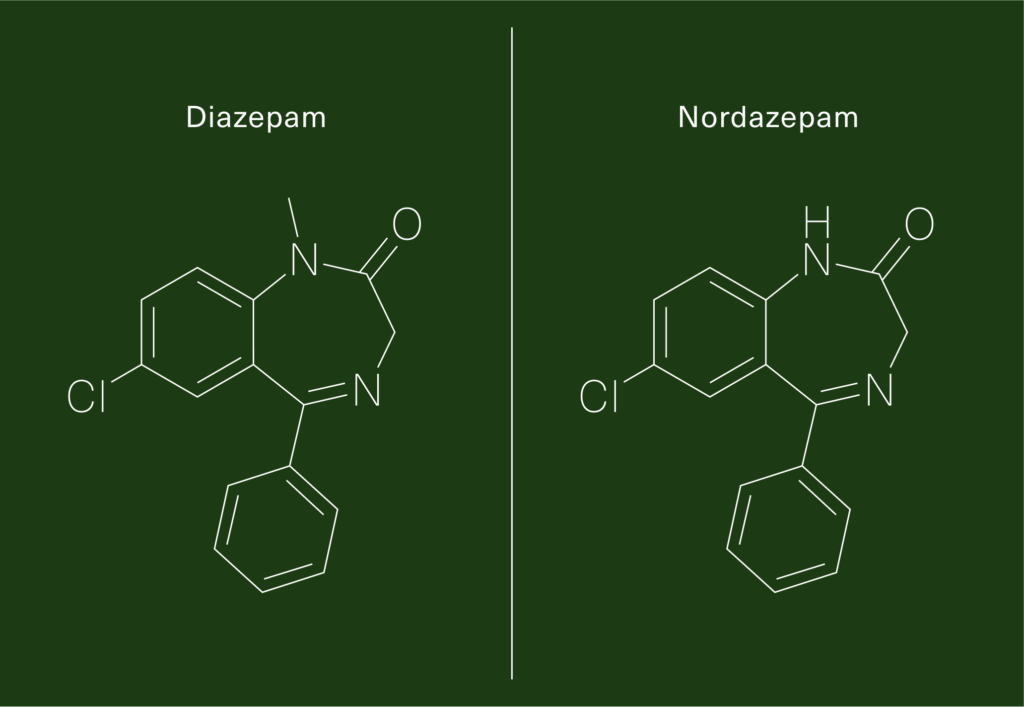
This was, in fact, a fair objection. There are some things that the human body simply doesn’t have the capacity to do, and organochlorine chemistry is one of them. Nowhere in the genome will you find enzymes that can take a chlorine atom and attach it to a carbon atom, the way it is in the structure of most benzodiazepines.
Nowhere in the human genome, anyway. But if you look in the gut microbiome, this vast and variable soup of alien biochemistry that we all carry around with us 24/7, you can find some features that might surprise you.
How the Gut Microbiome Makes The “Impossible” Possible
The final piece of the puzzle—or at least, the final piece that we have so far—dropped into place in 1995, with the publication of a paper by another group of researchers at the NIH.11 In it, they reported that they had identified a gut bacterium, Acinetobacter lwoffii, which was capable of elevating levels of benzodiazepine-like compounds in animals’ brains by producing a precursor—a molecule that’s inactive on its own, but gets converted to an active form once inside the brain.
Suddenly, there was a clean story: Certain gut bacteria produce this chemical, which the body wouldn’t be able to make on its own—probably because the synthesis involves attaching a chlorine atom to a carbon. The molecule gets absorbed into the bloodstream, and then converted by the brain into a natural regulator of GABA activity when it’s needed. When everything is working properly, the metabolic enzymes in your liver continuously clear this active molecule from the bloodstream as it comes out of the brain, keeping levels low. But if your liver shuts down, the compound starts to build up: Since it’s effectively being produced by a microbe and not your own body, there’s no built-in feedback control to halt its production. Once the levels get high enough, this sends you into a flumazenil-reversible coma, the same way taking a week’s worth of Valium at once would.
As an explanation for the findings up until that point, it was nice and neat.
But all of this research was done before the term “microbiome” was even coined—before DNA sequencing had gotten cheap enough to enable us to peer closely at the bacterial world inside, before we knew that many of the bacteria found in the mammalian gut are found nowhere else on Earth, and—crucially—before we knew that you can lose these bacteria if you’re not careful, sometimes with disastrous consequences.
Until we began to understand all this in the late 2000s, bacteria were viewed largely as either pathogens to be dispatched or as commensals—mostly harmless hitchhikers, whose presence or absence is generally inconsequential beyond the realm of digestion. As a result, the researchers who characterized the benzo-like activity from Acinetobacter lwoffii were focused largely on the known problem of what happens when you have too much of this bacterium’s benzodiazepine byproduct. They never seemed to give much consideration to the possibility that you could have too little.
What would it look like, if a person got unlucky with a course of antibiotics, and accidentally killed off the gut bacteria that had previously served as “in-house” factories, providing a slow-drip of natural benzodiazepines? Naturally, you might expect that person to need exogenous benzos—drugs from the pharmacy—to pick up the slack, in order to function normally. You might expect something that looks an awful lot like an anxiety disorder.
It’s a sobering prospect, but it’s also an exciting one. Maybe a cure for some people’s anxiety could be as simple as developing the right kind of probiotic—one that puts the “factory” back in the person where it belongs, to produce the necessary trace amounts of these compounds from the foods we eat every day.
Before you go looking for an Acinetobacter probiotic, it’s important to know that it’s an opportunistic pathogen that can cause everything from meningitis to pneumonia in susceptible people. So you’re unlikely to find it on shelves in the supplements aisle any time soon. Nevertheless, there’s reason to expect that Acinetobacter isn’t the only type of gut bug with this ability: The whole genus is characterized by a remarkable ability to vacuum up genes from its environment and put them to use.12 This tendency, coupled with the ever-growing abundance of antibiotic-resistance genes, can make them nasty pathogens—but at the same time, it means it’s all too possible that the strain identified as an endo-benzo precursor producer in that 1995 study picked up that ability from another microbe in the gut, which might be more generally friendly.
What we do know now is that you can support your gut-brain axis by abiding by many tried-and-true health guidelines. Eat a plant-rich diet, low in sugar, preservative agents, processed foods, food additives, and saturated fats. There’s also evidence that sleep and regular exercise can both affect the microbiome and the gut-brain connection.13,14
If that advice seems less satisfying than a probiotic cure that efficiently targets the root cause of anxiety, know that the scientific community is getting there. It’s taken decades to even identify that there is a gut-brain axis, and now we have a much wider knowledge base on which to continue our journey. With each discovery, we move closer to a world in which we can more precisely harness the power of probiotics to significantly alter our moods. In the meantime, as you (and your brain’s neurotransmitters) continue to experience the metaphorical “tastes” of life, it’s a good idea to nourish your gut and quite literally cook for yourself.
Citations
- Nuwer, R. (2014, January 7). Dolphins seem to use toxic pufferfish to get high. Smithsonian Magazine. https://www.smithsonianmag.com/smart-news/dolphins-seem-to-use-toxic-pufferfish-to-get-high-180948219/
- Sprouse-Blum, A. S., Smith, G., Sugai, D., & Parsa, F. D. (2010). Understanding endorphins and their importance in pain management. Hawaii medical journal, 69(3), 70–71.
- Bræstrup, C., & Squires, R. F. (1977). Specific benzodiazepine receptors in rat brain characterized by high-affinity (3H)diazepam binding. Proceedings of the National Academy of Sciences of the United States of America, 74(9), 3805–3809. https://doi.org/10.1073/pnas.74.9.3805
- Krogsgaard‐Larsen, P., & Arnt, J. (1980). Pharmacological studies of interactions between benzodiazepines and GABA receptors. Brain Research Bulletin, 5, 867–872. https://doi.org/10.1016/0361-9230(80)90146-x
- Campo-Soria, C., Chang, Y., & Weiss, D. S. (2006). Mechanism of action of benzodiazepines on GABAA receptors. British journal of pharmacology, 148(7), 984–990. https://doi.org/10.1038/sj.bjp.0706796
- Jones, E. A., Basile, A. S., & Skolnick, P. (1990). Hepatic encephalopathy, GABA-ergic neurotransmission and benzodiazepine receptor ligands. In Advances in Experimental Medicine and Biology (pp. 121–134). https://doi.org/10.1007/978-1-4684-5826-8_7
- Shoar, N. S. (2023, May 23). Flumazenil. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK470180/
- Pélissolo, A. (1995). [The benzodiazepine receptor: the enigma of the endogenous ligand]. PubMed, 21(2), 133–140. https://pubmed.ncbi.nlm.nih.gov/7781584
- Butterworth, R. F., & Layrargues, G. P. (1990). Benzodiazepine receptors and hepatic encephalopathy. Hepatology, 11(3), 499–501. https://doi.org/10.1002/hep.1840110323
- Klotz, U., & Walker, S. (1989). Flumazenil and hepatic encephalopathy. The Lancet, 333(8630), 155–156. https://doi.org/10.1016/s0140-6736(89)91165-3
- Yurdaydın, C., Walsh, T. J., Engler, H. D., Ha, J., Li, Y., Jones, E. A., & Basile, A. S. (1995). Gut bacteria provide precursors of benzodiazepine receptor ligands in a rat model of hepatic encephalopathy. Brain Research, 679(1), 42–48. https://doi.org/10.1016/0006-8993(95)00241-h
- Seitz, P., & Blokesch, M. (2013). Cues and regulatory pathways involved in natural competence and transformation in pathogenic and environmental Gram-negative bacteria. Fems Microbiology Reviews, 37(3), 336–363. https://doi.org/10.1111/j.1574-6976.2012.00353.x
- Shah, S., Mu, C., Moossavi, S., Shen-Tu, G., Schlicht, K., Rohmann, N., Geisler, C., Laudes, M., Franke, A., Züllig, T., Köfeler, H., & Shearer, J. (2023). Physical activity-induced alterations of the gut microbiota are BMI dependent. FASEB journal : official publication of the Federation of American Societies for Experimental Biology, 37(4), e22882. https://doi.org/10.1096/fj.202201571R
- Li, Y., Hao, Y., Fan, F., & Zhang, B. (2018c). The role of microbiome in insomnia, circadian disturbance and depression. Frontiers in Psychiatry, 9. https://doi.org/10.3389/fpsyt.2018.00669



