Diet is one of the most important levers of gut health. But sifting through all of the (sometimes conflicting) information out there is overwhelming. Here, we distill “eating for your gut” to a simple, but powerful, guiding principle.

Whether you’re swiping on Instagram, scrolling through TikTok, or following the headlines about gut health, the revolving door of nutrition advice can be head-spinning. Is gluten the enemy? Do I need a gut reset? And what the F are FODMAPs? Diet is one of the most flooded and overcomplicated landscapes to navigate. But it’s also one of the most important and impactful levers of our gut health, so learning how to effectively sift through all of the information out there is crucial to make informed decisions about what you consume each day.
And to be clear: “Gut health” does not just refer to digestion and symptoms like heartburn or bloating. The gut is an interconnected system that extends far beyond the boundaries of the gastrointestinal tract. At the core of this is your gut microbiome, which influences everything from immune function and cardiovascular health to mood. So “eating for your gut” is really about whole-body health, since the foods you eat are instrumental in shaping your microbial community.
Unfortunately, amid Internet echo chambers, commercialization of highly addictive processed foods, hyperbolic clickbait, and a diet culture tethered to restriction, it’s easy to lose sight of how to feed ourselves and our microbes. At Seed, we receive questions that reflect this dietary dilemma daily: What’s the healthiest diet for my microbiome? Which specific foods should I eat—or not eat—to support my gut? What’s the deal with [insert diet-of-the-week here]?
To bring some clarity—and science—to the conversation, we’ll start with a foundational question that will help guide you through this overwhelming space and give you the high-level information you need to nourish yourself and the microbes that call you home.

Science with us—nerdy reads for your inbox biome1
1By signing up, you consent to receive Seed emails.
What is the “best” diet for your gut?
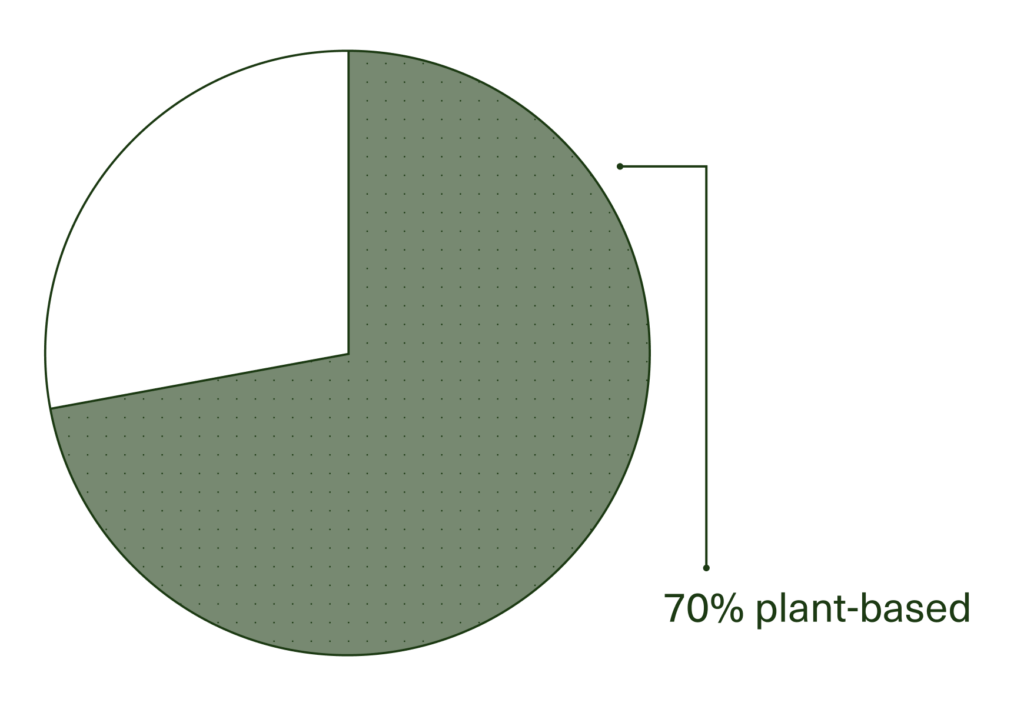
The short answer: Eat a high-fiber diet that’s 70% plant-based and includes fermented foods.
While this 70% number is a simplified high-level answer, it’s a key filter you can use to help make decisions about “eating for your gut.” If you find yourself confused or trying to sort through conflicting advice, it’s helpful to come back to this quick rule of thumb as the foundation for what you decide to consume. Read on for more specifics in the long answer. 🤓
The long answer: We can’t answer this question without considering the microbiome. Your gut microbiome has a profound impact on your gastrointestinal and overall health (for better or worse), so nurturing your microbial community is critical. One of the most meaningful ways to do this is through diet.
Every time you eat, countless microbial interactions take place along your gastrointestinal tract, directly influencing the community that resides within. Different microbes thrive on different dietary components (some are literally living for the carbs, others for the meat), so what you consume is a key factor in determining which microbes are present and in what proportions (a.k.a. “composition”). The outcomes of the interaction between food and your gut microbiome don’t end with digestion. A balanced and diverse microbial composition is key to overall health, and disruption to this balance (“dysbiosis”) is linked to many diseases, including inflammatory bowel disease (IBD), type 1 and type 2 diabetes, and autism.1
The gut microbiome responds rapidly—we’re talking 24 hours—to changes in diet.2 Although these changes are temporary, they may explain why you experience digestive discomforts like bloating, gas, diarrhea, or constipation when you alter your eating habits (while traveling, for instance). But quick shifts are not what matter in the long term: Sustained dietary patterns are the dominant force in determining the composition of your gut microbiome.3 So, back to the question at hand: What is the “best” diet for your gut?
As Dr. Emeran Mayer, gastroenterologist and member of Seed’s Scientific Board put it: “People tend to overcomplicate this topic, but it’s actually a fairly simple answer. The best diet is what’s best for your microbes. At a very high level, unless you have a particular deficiency or health condition, that can be any diet that is at least 70% plant-based and high in different types of fiber and fermented foods. So it doesn’t matter if your diet is vegetarian, Mediterranean, or paleo as long as you’re meeting that high-level criteria.”
Learn more from Dr. Emeran Mayer:
Looking for science-backed recipes to support your gut health? Dr. Mayer’s new cookbook Interconnected Plates offers practical tips and guidelines to translate the science of the gut-brain-microbiome axis into daily meals that optimize well-being. With over 55 easy-to-make recipes, it promotes health for the body, mind, and planet. Get cooking here.
Hungry for more? Learn the latest cutting-edge science on the root causes of IBS and IBS-like symptoms (and how to minimize or even eliminate them) in Dr. Mayer’s course: Take Charge of Your IBS Symptoms. Learn more here and use the code SEED at checkout for $200 off (valid through 12/31/25).
In addition to this foundational guideline, here are some specific science-backed recommendations to eat for your microbiome:
- Prioritize a diverse range of foods. Different microbes feed on different dietary components, so consuming a wide variety of fruits, vegetables, legumes, nuts, and grains can help support a more diverse microbial community, a primary indicator of gastrointestinal health.4
- Include an abundance of plant-derived compounds like fiber and polyphenols (naturally occurring compounds that typically act as antioxidants). Your gut microbes can ferment and transform these into metabolites that have a range of beneficial effects in the body. Short-chain fatty acids (SCFAs), for example, are produced when microbes break down insoluble fiber. Among their many roles, SCFAs act as nutrients for local colon cells, maintain intestinal barrier function and integrity, and provide protection against local inflammation.5 (Great sources include walnuts, pomegranate, berries, and green tea.)
- Incorporate Omega-3 and monounsaturated fats. These healthy fats can positively alter the gut microbiome and support growth of beneficial microbes, such as butyrate-producing bacteria.6 Butyrate is one of several short-chain fatty acids. (Great sources include salmon, avocados, olive oil, chia seeds, and pumpkin seeds.)
- Consider the ecological footprint of your food choices. The health implications of your diet go beyond the gut microbiome. Over-consuming foods with higher ecological footprints (such as red meat, dairy, and even off-season produce) will have a greater impact on climate change and the balance of ecosystems—which can take a major toll on human health. While removing animal products is a personal choice, consider replacing or complementing your meals with more locally sourced, plant-based options.
- Limit microbiome disruptors. Certain inputs contain compounds and chemicals that disrupt the gut, the gut barrier (the protective wall that lines your GI tract), and your microbes. Alcohol, for instance, has been shown to affect the composition of microbes in the gut, changing the proportions of beneficial and harmful bacteria, which can lead to dysbiosis.7 In addition to alcohol, be mindful of your intake of sugar, preservative agents, additives, and non-steroidal anti-inflammatory drugs (NSAIDs).
An important caveat to all of this: Diet affects people differently, because every person and their gut microbiome is unique, like an enormous living fingerprint. So, the foods you consume and how they make you feel are distinct and personal experiences that move between surviving and thriving. Just as there is no one universally healthy microbiome, there is no one-size-fits-all “perfect” diet.
As you navigate your way through the noisy space that is “eating for your gut,” look to these guidelines as your North Star, and you’ll be much less likely to lose your way.
Stay tuned for more answers to the top questions we receive about eating for your gut—from gluten intolerance and low FODMAPs, to the truth about gut “resets.”
Citations
- DeGruttola, A. K., Low, D., Mizoguchi, A., & Mizoguchi, E. (2016). Current Understanding of Dysbiosis in Disease in Human and Animal Models. Inflammatory bowel diseases, 22(5), 1137–1150. https://doi.org/10.1097/MIB.0000000000000750
- David, L. A., Maurice, C. F., Carmody, R. N., Gootenberg, D. B., Button, J. E., Wolfe, B. E., Ling, A. V., Devlin, A. S., Varma, Y., Fischbach, M. A., Biddinger, S. B., Dutton, R. J., & Turnbaugh, P. J. (2014). Diet rapidly and reproducibly alters the human gut microbiome. Nature, 505(7484), 559–563. https://doi.org/10.1038/nature12820
- Sonnenburg, J. L., & Bäckhed, F. (2016). Diet-microbiota interactions as moderators of human metabolism. Nature, 535(7610), 56–64. https://doi.org/10.1038/nature18846
- McDonald, D., Hyde, E. R., Debelius, J. W., Morton, J. P., González, A., Ackermann, G., Aksenov, A. A., Behsaz, B., Brennan, C., Chen, Y., Goldasich, L. D., Dorrestein, P. C., Dunn, R. R., Fahimipour, A. K., Embree, M., Gilbert, J. A., Gogul, G., Green, J. L., Hugenholtz, P., . . . Knight, R. (2018). American Gut: an Open Platform for Citizen Science Microbiome Research. MSystems, 3(3). https://doi.org/10.1128/msystems.00031-18
- Silva, Y. P., Bernardi, A., & Frozza, R. L. (2020b). The Role of Short-Chain Fatty Acids From Gut Microbiota in Gut-Brain Communication. Frontiers in Endocrinology, 11. https://doi.org/10.3389/fendo.2020.00025
- Costantini, L., Molinari, R., Farinon, B., & Merendino, N. (2017). Impact of Omega-3 Fatty Acids on the Gut Microbiota. International journal of molecular sciences, 18(12), 2645. https://doi.org/10.3390/ijms18122645
- Lee, E., & Lee, J. (2021b). Impact of drinking alcohol on gut microbiota: recent perspectives on ethanol and alcoholic beverage. Current Opinion in Food Science, 37, 91–97. https://doi.org/10.1016/j.cofs.2020.10.001