When you drink alcohol, your body embarks on a hero's journey to overcome the effects of imbibing. Here's how alcohol affects the microbiome and how you can support your gut in its fight to recover.

Bad news for those who enjoy drinking alcohol: As it turns out, imbibing can indeed affect your gut microbiome.
The good news? With a few simple measures, you can help lessen the negative impacts of alcohol and promote a thriving gut. Here, we’ll dive into what could be happening to your gut microbiome when you drink and provide suggestions for simple, research-informed steps toward restoring it.

Science with us—nerdy reads for your inbox biome1
1By signing up, you consent to receive Seed emails.
Remember: You Are a Unique Superorganism
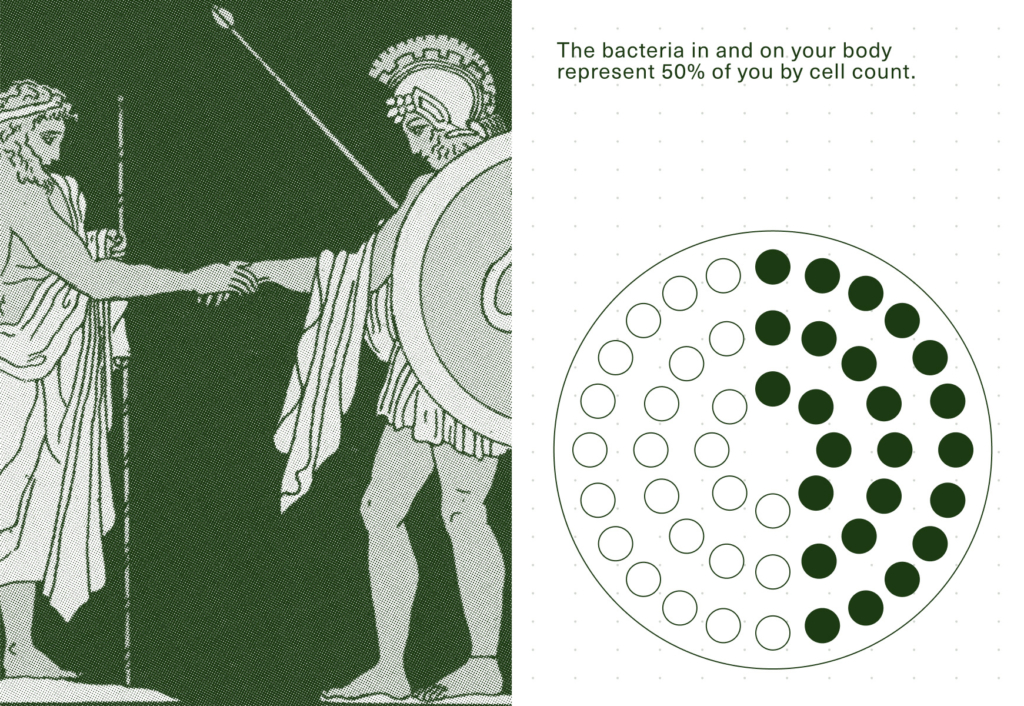
First things first: To tell the story of what happens to your gut microbiome when you drink alcohol, it’s important to remember that you (the protagonist in this story) are a Superorganism. And that’s not just a platitude. We know that a healthy gut is home to an abundance of microbes that support our well-being. In fact, our bodies are comprised of more than 38 trillion bacteria that live inside and among us, and they perform numerous functions that the human part of our biology can’t do on its own.1 Crucially, the microbiome isn’t set in stone: It’s flexible, shaped by external factors including the choices we make every day.2
This is all to say that you have agency when it comes to the health of your microbiome. When it comes to alcohol, emerging research is just beginning to articulate the precise ripple effects of drinking on our microbes, our bodies, and our health.3 Keep in mind that many such studies rely on animal models or long-term heavy drinking subjects, or use only ethanol (alcohol in its purest form, without the added flavors and sugars of the full drink). In other words, they often do not accurately reflect how most people drink, so take them with a grain of salt. Or a salted rim, if you will.
How Alcohol Affects the Microbiome—and Vice Versa
You may already know that alcohol can kill microbes. That’s why it’s used in many household cleaners, wound-care products, hand sanitizers, and other solutions for wiping out bacteria. But it actually takes a pretty high concentration of alcohol to kill microbes—higher than you’re likely to find in the gut after drinking, unless you’re doing shots. Even then, alcohol is diluted by mixing with the contents of your stomach (assuming you’re not drinking on an empty stomach), then mostly absorbed in the small intestine, well “upstream” of where the majority of our gut flora live.4 The interaction between alcohol and bacteria is a two-way street, though: A 2001 study found that bacteria in the mouth can turn alcohol into the carcinogen acetaldehyde, and that poor dental health can roughly double your exposure to this toxic metabolite (all the more reason to brush your teeth before bed after a night out).5
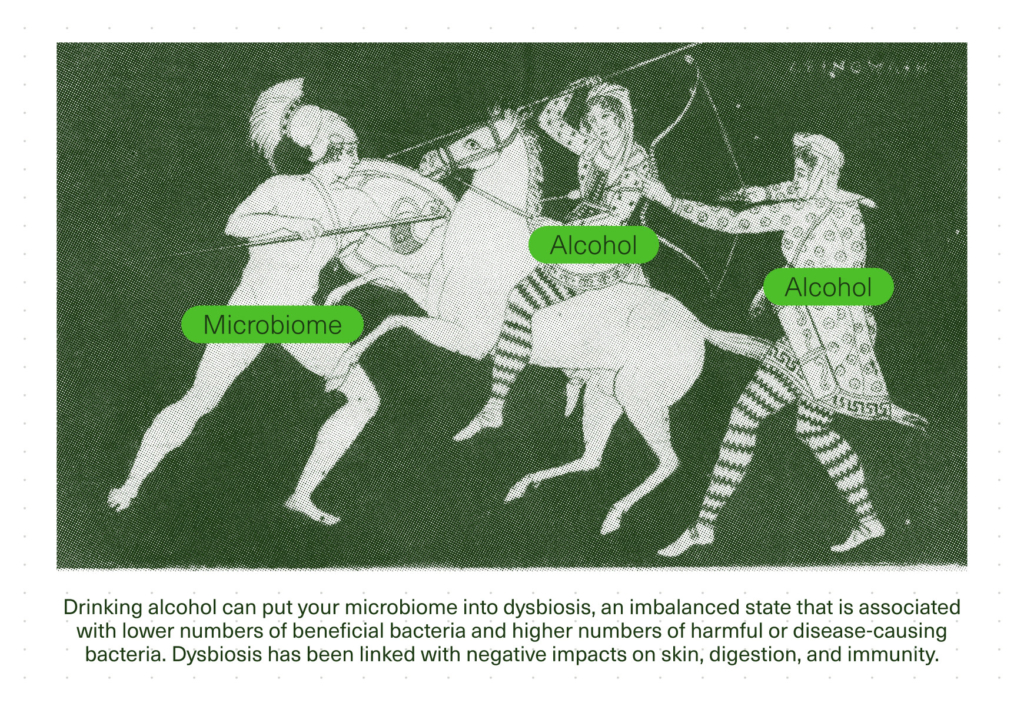
Even if it’s not directly killing gut bacteria, alcohol has been shown to affect the composition of microbiota in the gut, changing the proportions of beneficial and pathogenic bacteria.6 This can lead to what’s called a “dysbiotic state,” or “dysbiosis,” an imbalanced state that is associated with lower numbers of beneficial bacteria and higher numbers of harmful or disease-causing bacteria. Dysbiosis has also been linked with negative impacts on our skin, immunity, and digestion—all key indicators of good health.7,8
The jury’s still out on exactly how alcohol consumption can lead to gut dysbiosis. According to Sherri Simmons, PhD, Vice President of Discovery at Seed Health, more work is needed to decipher the interactions between alcohol, microbes, and impacts on gut health. But there are a couple of plausible hypotheses:
- Processing alcohol may change the availability of microbes’ favorite foods. Essentially, processing alcohol can yield chemicals that affect the food that’s available for our microbes. Ethanol, for example, is a low-energy food for microbes, and microbes tend to consume more nutrient-rich foods when they’re available. Shifts in their favorite energy sources can lead to changes in the overall microbiome. In terms of how the gut is impacted after drinking, it was originally thought that gut microbes metabolize ethanol directly, leading to dysbiosis. But a recent study in mice suggests this may not be the case, and that microbes are actually responding to increased levels of acetate (better known as vinegar), a product of alcohol metabolism in our own cells.9 (Other studies have shown that certain bacteria can ferment ethanol directly in vitro to produce acetaldehyde, but this is not yet shown to be a significant process in our guts.)10
- Drinking alcohol could trigger SIBO. Heavy alcohol consumption is associated with bacterial overgrowth in the small intestine, a condition known as “SIBO.”11 A healthy small intestine has relatively few bacteria compared to the large intestine, and this overgrowth can contribute to increased intestinal permeability—meaning that bacteria and bacterial byproducts translocate outside the gut and can contribute to inflammation and liver damage.
Dr. Simmons posits that these processes are not mutually exclusive. In fact, it’s possible both are happening simultaneously. In addition to contributing to a dysbiotic state, alcohol has been shown to compromise the gut barrier, specifically the epithelial cells lining the small intestine.12 These cells are your gut’s gatekeepers that “decide” what goes into the bloodstream from the small intestine and what does not. Ongoing research has connected damaged epithelial cells to bacterial overgrowth and an increase in pro-inflammatory cytokines (proteins that mediate immune system function).13,14
EXPLORE FURTHER: Why Does Alcohol Make You Poop?
The Liver: Not Just a Supporting Character
Then, of course, there’s alcohol’s impact on the liver. Many people know that alcohol negatively impacts the liver, but you might not be aware that the liver plays an absolutely critical role in maintaining a healthy gastrointestinal (GI) tract. Bile salts, which are secreted by the liver and gallbladder in the small intestine, are key in limiting bacterial growth in this region of the digestive tract. When the liver is damaged from alcohol, its ability to secrete those bile salts into the small intestine is inhibited—which can introduce problems. As we discussed above, the small intestine is supposed to be relatively sparse in terms of its bacterial population: It’s the first part of the GI tract after the stomach, and it’s where we absorb a lot of nutrients like fat and simple carbohydrates from our food.
What we don’t absorb in the small intestine, like fiber, gets passed on to the large intestine, where your gut bacteria feast on that fiber and ferment it into short-chain fatty acids (SCFAs) and other beneficial compounds. The large intestine is built to safely house that fermentation process and absorb its useful byproducts, without letting any bits of the actual bacteria seep through into the bloodstream—but the small intestine isn’t. If microbes start blooming too early in the digestive process, bacterial proteins and other proinflammatory molecules can get absorbed, sending your immune system into red-alert mode.

Keeping things moving is also crucial. The small intestine is long (~22 feet), and if things stagnate for too long, this can predispose you to digestive issues like diverticulitis or SIBO. Unfortunately, alcohol can also affect motility in the small intestine, causing slower stool transit and more bacterial growth in a region of the GI tract that’s designed more for absorption than for fermentation.15
All in all, this sets the stage for a vicious cycle, wherein alcohol damages the liver, impairs bile secretion, and slows motility—all of which can alter the microbiome and contribute to dysbiosis. Because the liver is your body’s “first pass” filter for things passing from your GI tract into the bloodstream, this process predisposes the liver to further damage.
How to Support Your Gut
So to review: Exposure to alcohol can lead to a dysbiotic gut, which is associated with negative outcomes for our well-being. What can you do about it?
As we said, the choices you make every day impact your microbiome. Here are some ways you can support your gut if you drink alcohol:
- When you do drink, do so in moderation. We know there are documented health risks to drinking in excess, though some researchers believe that low-to-moderate alcohol consumption may actually have a protective effect on health outcomes like cardiovascular disease, diabetes mellitus, and mortality (a.k.a. death).16 However, this research is mostly observational, and conclusive evidence cannot be drawn about “healthy levels” of alcohol consumption based on associations alone.17 (For the record, “moderate” alcohol consumption is defined as one U.S. glass, or 14 g alcohol, per day for women and two U.S. glasses, or 28 g alcohol, per day for men.)
- Commit to a “dry” month. “Dry January” is not just a self-improvement gimmick. Research from 2014 shows a significant correlation between abstaining from alcohol and a healthier microbiome for alcohol-dependent individuals, which suggests that any kind of abstinence may help bolster microbial health.18
- Take a probiotic with prebiotics after drinking. Certain probiotic strains can promote a healthy gut environment, support microbial balance, and help the gut barrier recovery from occasional GI stressors.
- Eat a diet high in fiber. If you’re not living with Inflammatory Bowel Disease (IBD), a high-fiber diet can help feed SFCA-producing microbes, which are linked to lower levels of inflammation in the gut. Think: nuts, fruits, and veggies—superfoods for the “good” microbes.
- Order a glass of red. Microbes love polyphenols, and red wine is full of them. This study suggests that the polyphenols in red wine may contribute to a more diverse microbial community.19
So there you have it. The twists and (intestinal) turns have led us to the end of our story and its moral: If you choose to drink, it’s recommended that you do so in moderation, and then do what you can to support your gut microbiome.
Citations
- Sender, R., Fuchs, S., & Milo, R. (2016). Revised Estimates for the Number of Human and Bacteria Cells in the Body. PLOS Biology, 14(8), e1002533. https://doi.org/10.1371/journal.pbio.1002533
- Valdes, A. M., Walter, J., Segal, E., & Spector, T. D. (2018). Role of the gut microbiota in nutrition and health. BMJ, k2179. https://doi.org/10.1136/bmj.k2179
- Pohl, K., Moodley, P., & Dhanda, A. D. (2021). Alcohol’s Impact on the Gut and Liver. Nutrients, 13(9), 3170. https://doi.org/10.3390/nu13093170
- Levitt, M. D., Li, R., DeMaster, E. G., Elson, M., Furne, J., & Levitt, D. G. (1997). Use of measurements of ethanol absorption from stomach and intestine to assess human ethanol metabolism. The American journal of physiology, 273(4), G951–G957. https://doi.org/10.1152/ajpgi.1997.273.4.G951
- Homann, N., Tillonen, J., Rintamäki, H., Salaspuro, M., Lindqvist, C., & Meurman, J. H. (2001). Poor dental status increases acetaldehyde production from ethanol in saliva: a possible link to increased oral cancer risk among heavy drinkers. Oral oncology, 37(2), 153–158. https://doi.org/10.1016/s1368-8375(00)00076-2
- Lee, E., & Lee, J. (2021). Impact of drinking alcohol on gut microbiota: recent perspectives on ethanol and alcoholic beverage. Current Opinion in Food Science, 37, 91–97. https://doi.org/10.1016/j.cofs.2020.10.001
- Carding, S., Verbeke, K., Vipond, D. T., Corfe, B. M., & Owen, L. J. (2015). Dysbiosis of the gut microbiota in disease. Microbial ecology in health and disease, 26(0), 26191. https://doi.org/10.3402/mehd.v26.26191
- Salem, I., Ramser, A. E., Isham, N., & Ghannoum, M. A. (2018). The Gut Microbiome as a Major Regulator of the Gut-Skin Axis. Frontiers in Microbiology, 9. https://doi.org/10.3389/fmicb.2018.01459
- Martino, C., Zaramela, L. S., Gao, B., Embree, M., Tarasova, J., Parker, S. J., Wang, Y., Chu, H., Chen, P., Lee, K., Galzerani, D. D., Gengatharan, J. M., Lekbua, A., Neal, M. L., Knight, R., Tsukamoto, H., Metallo, C. M., Schnabl, B., & Zengler, K. (2022). Acetate reprograms gut microbiota during alcohol consumption. Nature Communications, 13(1). https://doi.org/10.1038/s41467-022-31973-2
- Tsuruya, A., Kuwahara, A., Saito, Y., Yamaguchi, H., Tsubo, T., Suga, S., Inai, M., Aoki, Y., Takahashi, S., Tsutsumi, E., Suwa, Y., Morita, H., Kinoshita, K., Totsuka, Y., Suda, W., Oshima, K., Hattori, M., Mizukami, T., Yokoyama, A., . . . Nakayama, T. (2016). Ecophysiological consequences of alcoholism on human gut microbiota: implications for ethanol-related pathogenesis of colon cancer. Scientific Reports, 6(1). https://doi.org/10.1038/srep27923
- Zhong, W., & Zhou, Z. (2014). Alterations of the gut microbiome and metabolome in alcoholic liver disease. World journal of gastrointestinal pathophysiology, 5(4), 514–522. https://doi.org/10.4291/wjgp.v5.i4.514
- Wang, Y., Tong, J., Chang, B., Wang, B., Zhang, D., & Wang, B. (2014). Effects of alcohol on intestinal epithelial barrier permeability and expression of tight junction-associated proteins. Molecular Medicine Reports, 9(6), 2352–2356. https://doi.org/10.3892/mmr.2014.2126
- Schnabl, B., & Brenner, D. A. (2014). Interactions between the intestinal microbiome and liver diseases. Gastroenterology, 146(6), 1513–1524. https://doi.org/10.1053/j.gastro.2014.01.020
- Mcc, C., N, L., Ferreira, C. R., Gonçalves, J., Almeida, D. B., Gamba, C., Cassali, G. D., Pedroso, S. H. S. P., Moreira, C., Martins, F., Nicoli, Teixeira, M. J., Alb, G., & Vieira, A. T. (2014). Comparing the effects of acute alcohol consumption in germ-free and conventional mice: the role of the gut microbiota. BMC Microbiology, 14(1). https://doi.org/10.1186/s12866-014-0240-4
- Grad, S., Abenavoli, L., & Dumitrascu, D. L. (2016). The Effect of Alcohol on Gastrointestinal Motility. Reviews on Recent Clinical Trials, 11(3), 191–195. https://doi.org/10.2174/1574887111666160815103251
- Drinking Levels Defined | National Institute on Alcohol Abuse and Alcoholism (NIAAA). (n.d.). https://www.niaaa.nih.gov/alcohol-health/overview-alcohol-consumption/moderate-binge-drinking
- Hendriks, H. F. J. (2020). Alcohol and Human Health: What Is the Evidence? Annual Review of Food Science and Technology, 11(1), 1–21. https://doi.org/10.1146/annurev-food-032519-051827
- Leclercq, S., Matamoros, S., Cani, P. D., Neyrinck, A. M., Jamar, F., Stärkel, P., Windey, K., Tremaroli, V., Bäckhed, F., Verbeke, K., de Timary, P., & Delzenne, N. M. (2014). Intestinal permeability, gut-bacterial dysbiosis, and behavioral markers of alcohol-dependence severity. Proceedings of the National Academy of Sciences of the United States of America, 111(42), E4485–E4493. https://doi.org/10.1073/pnas.1415174111
- Roy, C. I. L., Wells, P. M., Si, J., Raes, J., Bell, J. T., & Spector, T. D. (2019). Red Wine Consumption Associated With Increased Gut Microbiota α-Diversity in 3 Independent Cohorts. Gastroenterology, 158(1), 270-272.e2. https://doi.org/10.1053/j.gastro.2019.08.024



