Digestion is a vital process, and a healthy digestive system is important not only to overall gut health, but also to the health of your entire body.

For many, digestion occurs unconsciously as we go about our day and as we sleep. But if you’re reading this as someone whose digestive health is disruptive to your day-to-day life—you’re not alone.
Digestive problems are among the most prevalent health issues. In the US, for instance, nearly two-thirds of Americans have reported dealing with digestive issues,¹ some 50 million Americans experience chronic constipation,² and almost 15% of the US population suffers from Irritable Bowel Syndrome (IBS).³
So, what impacts digestive health? Before diving into the factors that influence your digestion and ways to support healthy function, let’s begin with an overview of what this system is and how it operates.
The digestive system is responsible for breaking down complex foods into accessible nutrients your body can use for energy, growth, and repair.
When we talk about digestive health, we’re referring to the proper functioning of this system. But, as many of us experience, digestive health is complex. There are many moving parts and the process doesn’t always run smoothly, which can lead to issues like gas, bloating, constipation, heartburn, and other debilitating discomforts. Like a machine, the digestive system requires regular care and maintenance.
So, how does digestion work?
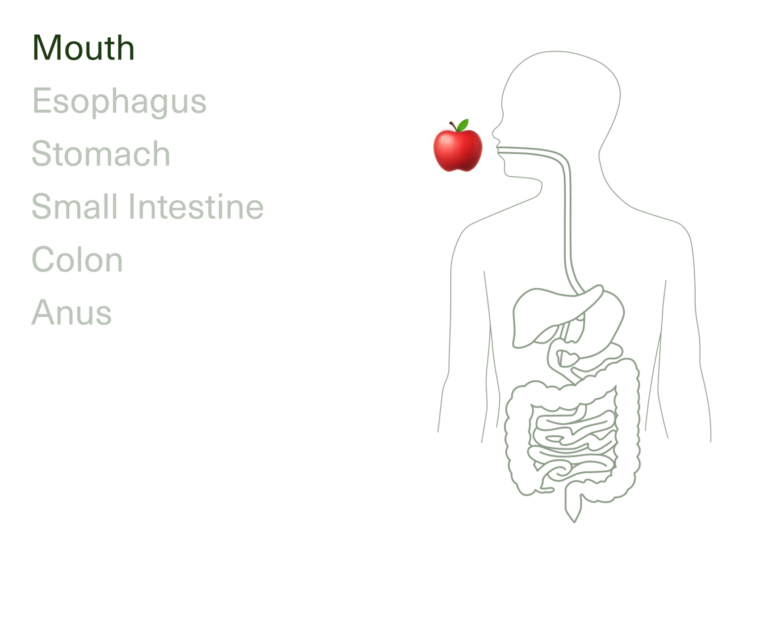
The journey of digestion begins in your mouth and the process continues through the esophagus, stomach, small intestine, large intestine, rectum, and anus. Together, these make up your gastrointestinal (GI) tract—a 30-foot tube that plays host to the world passing through (foods, liquids) and is home to your resident microbes. Nerves and hormones also play a major role in digestion by controlling the various steps throughout the process.
Upon entering the mouth, your teeth start breaking food down into smaller, more manageable pieces and saliva contains enzymes that break down starches. After swallowing, a process called peristalsis (muscle movement that helps push things along) kicks in and the food travels down toward the esophageal sphincter, to your stomach. In the stomach, digestive enzymes and stomach acids continue the breakdown that began in your mouth, and partially digested food, called chyme, is released into the small intestine.
Along this pathway, nutrients are absorbed. The leftover material is shipped off to the large intestine (or colon), where trillions of bacteria continue the process of breaking down what your body couldn’t. These are mostly fibers and other non-digestible carbohydrates. Your resident microbes also transform some of these compounds into secondary metabolites like short-chain fatty acids (SCFAs), which play a role in gut-brain interactions. Any additional nutrients, including water, are absorbed in the large intestine, and the remaining waste is expunged.
There are a lot of steps in this process where things can go wrong, and dealing with these mishaps can be overwhelming, frustrating, and even embarrassing, especially when it comes to talking about one of the key components of digestive health: your poop. And while there is no one-size-fits-all regimen for digestive health, there are some simple ways to take care of the digestive system on a daily basis.
(Note: these suggestions are not meant to supplement medical intervention, or treat any kind of digestive disease or condition.)
1. Diet
While there is no “perfect” diet, generally a healthy diet to support your digestive system and overall health contains the following:
- An abundance of diverse sources of plant fibers and polyphenols. These are found in vegetables, walnuts, berries, and green tea.4
- Adequate fiber.5 The National Institute of Medicine recommends about 25 grams for women and 38 grams for men.6
- Omega-3 fatty acids and monounsaturated fat. These are found in salmon, sardines, avocados, and olive oil.
- Limited sugar, preservative agents, processed foods, and/or food additives.
2. Hydration
Water is important to keep your inputs moving through your intestines. It’s also a critical component of stool itself, as poop is around 75% water,7 unless you’re experiencing diarrhea.
Inadequate fluid intake can cause stools to become dehydrated and difficult to pass—and can be a leading contributor to constipation.8
3. Exercise
Exercise can reduce colonic transit time (how quickly food passes through the digestive system), possibly due in part to hormonal changes during physical activity.9 Additionally, regular exercise may reduce symptoms of constipation,10 and can also help reduce inflammation within the gut, which may be beneficial in preventing certain digestive diseases.11
4. Support your microbiome
Your resident gut microbes help you digest food, synthesize key vitamins and nutrients, and even play a role in managing immune responses. Dysbiosis in the gut (i.e. an imbalance in the composition of the microbiome) has been linked to a host of gastrointestinal diseases and disorders, from constipation12 to inflammatory bowel disease,13 and even to gastric14 and colorectal cancer.15 Because the gut microbiome is intertwined with digestion, actions that support digestive health (such as those mentioned above) can also help support your microbiome and vice versa.
Beyond factors like diet and hydration, specific probiotics can also make a meaningful impact on digestive health.
Many people connect probiotics with gut and digestive health—and for good reason. Digestive and GI health are the most common (and researched) benefits associated with specific probiotic strains.
This is one of the questions we receive most frequently, often from individuals looking for probiotics to help with a variety of digestive concerns, from bloating to constipation.
Probiotics have been studied extensively to address gastrointestinal discomforts. For instance, in one study, researchers discovered specific strains that supported gastrointestinal functions: bowel movement regularity, stool consistency, ease of expulsion, bowel movement comfort, and ease of occasional bloating.16
When it comes to probiotics, benefits are assessed at the strain level and each unique strain can impart an array of beneficial effects. Therefore, if you’re turning to probiotics to support a particular aspect of digestion, it’s important to look for strains that have been clinically studied to demonstrate that health benefit you’re seeking, and are included in the probiotic you choose in the clinically relevant doses. For tips on choosing a probiotic: see here.
It’s also important to note: the US Food and Drug Administration (the FDA) categorizes probiotics as dietary supplements and regulates them as such. As a dietary supplement, probiotic products should not claim to diagnose, treat, cure, or prevent any disease or condition. That said, probiotics hold great promise for future alternative and supportive therapies, and this field is continuing to grow as the scientific and clinical research expands.
While digestion is one of the most complex systems in the human body, we’re at a pivotal (and hopeful) moment in how we approach digestive health—and treat and care for those experiencing digestive disease.
Growing interest, inquiry, and research surrounding the microbiome (and areas like the gut-brain axis) are expanding our knowledge of digestive health, and opening the door for novel solutions to some of the most pervasive digestive health issues we’re facing. From the development of microbial therapeutics to fecal transplants to new probiotic applications, we’re ushering in a new era of digestive health.
- Almario, C. V., Ballal, M. L., Chey, W. D., Nordstrom, C., Khanna, D., & Spiegel, B. M. R. (2018b). Burden of Gastrointestinal Symptoms in the United States: Results of a Nationally Representative Survey of Over 71,000 Americans. American Journal of Gastroenterology, 113(11), 1701–1710. https://doi.org/10.1038/s41395-018-0256-8
- Oh, S. J., Fuller, G., Patel, D., Khalil, C., Spalding, W., Nag, A., Spiegel, B. M. R., & Almario, C. V. (2020). Chronic Constipation in the United States: Results From a Population-Based Survey Assessing Healthcare Seeking and Use of Pharmacotherapy. American Journal of Gastroenterology, 115(6), 895–905. https://doi.org/10.14309/ajg.0000000000000614
- Irritable Bowel Syndrome. (2022, March 21). American College of Gastroenterology. https://gi.org/topics/irritable-bowel-syndrome/#tabs3
- McDonald, D., Hyde, E., Debelius, J. W., Morton, J. T., Gonzalez, A., Ackermann, G., Aksenov, A. A., Behsaz, B., Brennan, C., Chen, Y., DeRight Goldasich, L., Dorrestein, P. C., Dunn, R. R., Fahimipour, A. K., Gaffney, J., Gilbert, J. A., Gogul, G., Green, J. L., Hugenholtz, P., Humphrey, G., … Knight, R. (2018). American Gut: an Open Platform for Citizen Science Microbiome Research. mSystems, 3(3), e00031-18. https://doi.org/10.1128/mSystems.00031-18
- Anderson, J. W., Baird, P., Davis, R. H., Jr, Ferreri, S., Knudtson, M., Koraym, A., Waters, V., & Williams, C. L. (2009). Health benefits of dietary fiber. Nutrition reviews, 67(4), 188–205. https://doi.org/10.1111/j.1753-4887.2009.00189.x
- Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids. (2005). Institute of Medicine. https://doi.org/10.17226/10490
- Rose, C., Parker, A., Jefferson, B., & Cartmell, E. (2015). The Characterization of Feces and Urine: A Review of the Literature to Inform Advanced Treatment Technology. Critical reviews in environmental science and technology, 45(17), 1827–1879. https://doi.org/10.1080/10643389.2014.1000761
- Forootan, M., Bagheri, N., & Darvishi, M. (2018). Chronic constipation. Medicine, 97(20), e10631. https://doi.org/10.1097/md.0000000000010631
- Huang, R., Ho, S. Y., Lo, W. S., & Lam, T. H. (2014). Physical Activity and Constipation in Hong Kong Adolescents. PLoS ONE, 9(2), e90193. https://doi.org/10.1371/journal.pone.0090193
- Oettle, G. J. (1991). Effect of moderate exercise on bowel habit. Gut, 32(8), 941–944. https://doi.org/10.1136/gut.32.8.941
- Bilski, J., Brzozowski, B., Mazur-Bialy, A., Sliwowski, Z., & Brzozowski, T. (2014). The role of physical exercise in inflammatory bowel disease. BioMed research international, 2014, 429031. https://doi.org/10.1155/2014/429031
- Ohkusa, T., Koido, S., Nishikawa, Y., & Sato, N. (2019). Gut Microbiota and Chronic Constipation: A Review and Update. Frontiers in medicine, 6, 19. https://doi.org/10.3389/fmed.2019.00019
- Valdes, A. M., Walter, J., Segal, E., & Spector, T. D. (2018b). Role of the gut microbiota in nutrition and health. BMJ, k2179. https://doi.org/10.1136/bmj.k2179
- Park, J. Y., Seo, H., Kang, C. S., Shin, T. S., Kim, J. W., Park, J. M., Kim, J. G., & Kim, Y. K. (2022). Dysbiotic change in gastric microbiome and its functional implication in gastric carcinogenesis. Scientific Reports, 12(1). https://doi.org/10.1038/s41598-022-08288-9
- Cheng, Y., Ling, Z., & Li, L. (2020). The Intestinal Microbiota and Colorectal Cancer. Frontiers in Immunology, 11. https://doi.org/10.3389/fimmu.2020.615056
- del Piano, M., Carmagnola, S., Anderloni, A., Andorno, S., Ballarè, M., Balzarini, M., Montino, F., Orsello, M., Pagliarulo, M., Sartori, M., Tari, R., Sforza, F., & Capurso, L. (2010b). The Use of Probiotics in Healthy Volunteers With Evacuation Disorders and Hard Stools. Journal of Clinical Gastroenterology, 44(Supplement 1), S30–S34. https://doi.org/10.1097/mcg.0b013e3181ee31c3



